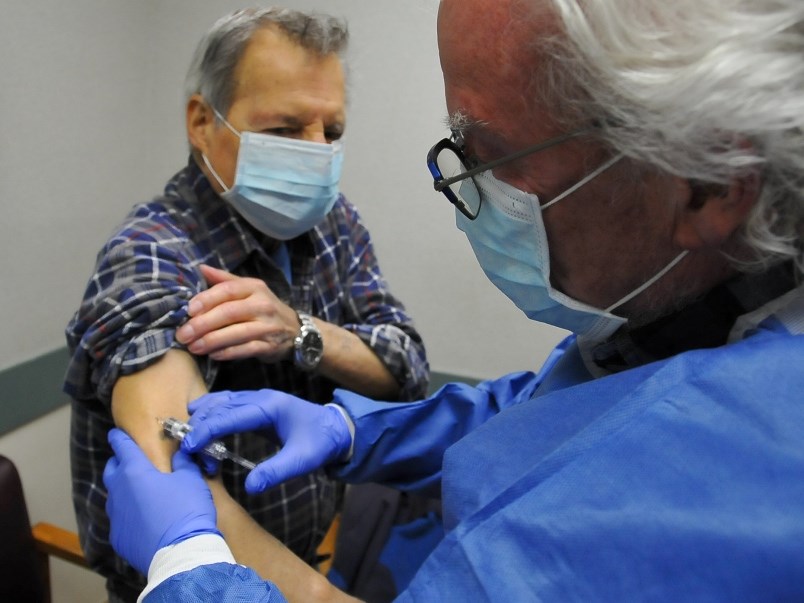
More than one in five Canadian adults report having no family doctor, a new study has found.
The analysis is based on survey responses from more than 9,200 people across 乌鸦传媒, collected in the fall of 2022 and in the Canadian Medical Association Journal Tuesday by 21 doctors and medical researchers from across the country.
First author Dr. Tara Kiran, a family physician at St. Michael’s Hospital and associate professor at the University of Toronto, said its unconscionable that in some parts of the country, a third of adults — about 6.5 million Canadians — are shut out from access to regular primary health care.
“The degree of provincial variation was surprising,” said Kiran. “We have one country and this study really speaks to how we have 14 different health systems.”
The results also showed big regional gaps in primary care. In British Columbia, 28 per cent of residents said they didn’t have regular access to a family physician, while in Quebec and Atlantic 乌鸦传媒, that number rose to 31 per cent. Men, people under 65, and those with poor self-reported health problems were also less likely to report having a family doctor.
“If you are in 乌鸦传媒, if you compare yourself to people living in Ontario, you’re much less likely to have a family doctor or nurse practitioner,” said Kiran.
Goldis Mitra, a family doctor in North Vancouver and researcher at UBC, said that every week she gets at least 20 people calling or asking her personally to help find a family doctor.
“If you're stretched too thin, you can't provide patients with the care that you know they need,” said Mitra, who also co-authored the study.
“But at the same time, you worry about the patients who aren't able to access care at all. And isn't any care better than no care? It's a really challenging predicament.”
Walk-in clinic use highest in 乌鸦传媒
Almost half of those who took part in the survey reported visiting a walk-in clinic once or more in the 12 months before they filled out the 15-minute survey.
Canadians who had the highest odds of visiting a walk-in clinic included women, young adults, people outside of rural areas, and those with poor or fair health. More than any other province, simply living in 乌鸦传媒 raised the odds someone would visit a walk-in clinic, the study found.
“The biggest difference in walk-in clinic use was between those who did and those who did not have a primary care clinician,” the report said.
The study comes as many countries around the world work to reform their public health-care systems in the face of aging populations, greater inequality, and a rising prevalence of mental health and addictions problems, the study says.
The COVID-19 pandemic made the situation in 乌鸦传媒 even worse as many family physicians opted for early retirement, note the authors. Existing research also shows that burnout is driving others to seek a similar path in the coming years.
“Even before the COVID-19 pandemic, people in 乌鸦传媒 reported some of the worst access to primary care among high-income countries,” says the study.
The study found even those who have a family doctor are struggling to get care during the evenings and weekends. Kiran said 36 per cent of people struggled to see their family doctor outside of standard work hours.
One of the clearest messages from the study shows Canadians care deeply about knowing their doctor as a person, said Kiran.
“We see people in 乌鸦传媒 want relationship-centred primary care, yet at the same time so many of them don't have that option and are turning to walk in presumably because they're the one place that people can get any care,” she said.
The study is latest in a 16-month national public engagement project on the future of the country's primary health-care system. Yet the authors warned it only painted a partial picture of gaps in family health care across 乌鸦传媒.
Among the study’s limitations, the authors say they had no responses from 乌鸦传媒’s territories and low response rates among new Canadians, racialized people, and those who identify as Indigenous. Those are the groups “we know are less likely to receive high-quality primary care,” the authors write.
Some suggest lack of doctors not the problem
Why so many Canadians don't have a family doctor has prompted governments across the country to scramble for answers. In a poll from the , roughly 900,000 British Columbians did not have a family doctor by April 2022. Of those, two-thirds said it’s because they “can’t find one,” and 19 per cent said they have lost their family doctor to closed practices.
In October 2022, the 乌鸦传媒 government introduced a new payment model to recruit and retain more family doctors in the province. By the end of 2023, 5,000 family doctors were working in long-term primary care, 708 more than the year earlier, according to the Ministry of Health.
The numbers have prompted some to seek answers to the doctor shortage outside of the health-care system. A February 2024 from the group Generation Squeeze found there were 141 family doctors per 100,000 British Columbians in 2022, up from 73 per 100,000 in 1976. The study also found federal dollars were increasingly filling in provincial gaps in social and education spending.
Paul Kershaw, founder of Generation Squeeze and a researcher at the UBC School of Population and Public Health, said at the time that “the truth may sound stranger than fiction,” but 乌鸦传媒 now has more doctors than ever, even after factoring in population growth.
The solutions, as he put it in the report, require investing in people's health before they land at the doctor and “are found in our neighbourhoods, jobs, child care centres and schools – something the pandemic made painfully clear.”
Roles of family doctors have changed
Mitra acknowledged the number of family doctors in 乌鸦传媒 has gone up since the 1970s. But she said the job has also changed.
“Not only do they work in your traditional family practice office, they work in the hospital providing inpatient care, they do palliative care, they deliver babies, they work in long-term care facilities, but also they do areas of much needed focused practice like sports medicine, emergency medicine,” Mitra said.
Many family doctors don’t end up in community clinics, and those that do are faced with a growing amount of paperwork as medicine becomes more complex. Compared to 20 years ago, Mitra said today there’s a much broader set of risk factors, as well as tests and medication that need to be considered. That all means more time and more resources are spent on each patient.
The solution, Mitra said, requires help from the 乌鸦传媒 government to reduce paperwork, improve electronic medical records and help family practices “make team-based care work in this province.”
“What we’re seeing play out is we just don’t have enough family doctors to do the work,” she said.